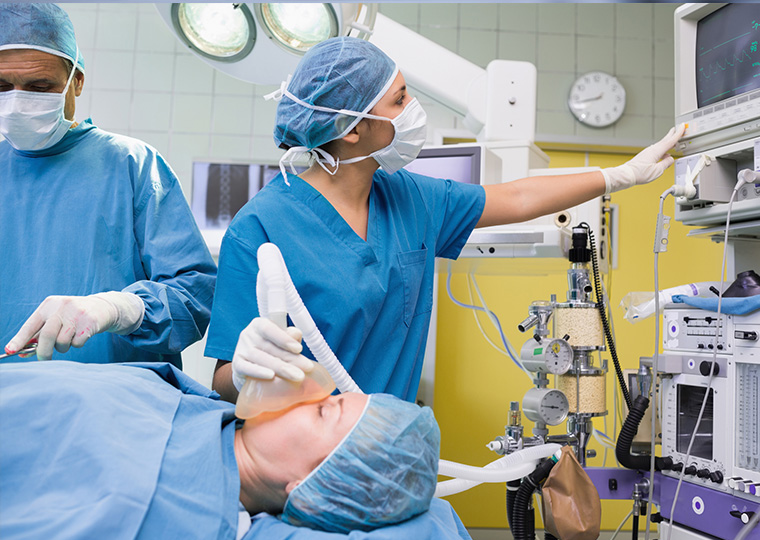
A model for staffing O.R.s incorporates the costs of worker dissatisfaction and idle time
Staffing hospital operating rooms is a tricky job with high stakes for everyone involved. Coordinators must make schedules long before knowing exactly how many surgeries will be performed, which specialists will be needed and how long each procedure will last. Miscalculations lead to disgruntled employees, higher health care costs generally and, in worst cases, patients without needed care.
From hospitals to retailers, employers routinely use algorithms — model-based systems — to set employee schedules that minimize direct costs, such as overtime expenses. But most employers routinely adjust computer-generated schedules by hand in order to keep employees happy. Scheduling complaints are high on the list of reasons employees leave for other jobs, and the price of frequent staff turnover isn’t included in standard staffing models.
A model that captures the hidden costs of staffing decisions that human schedulers are typically left to manage can significantly reduce operating room staffing costs, University of North Carolina’s Sandeep Rath and UCLA Anderson’s Kumar Rajaram find. Their model, demonstrated by assigning anesthesiologists across four subspecialties to operating rooms at Ronald Reagan UCLA Medical Center, is described in a study forthcoming in the journal Production and Operations Management.
Scheduling Software Identifies Explicit Costs but not Implicit Costs
The study focuses on management of the reserve (on-call) pool of anesthesiologists, which at UCLA Medical Center is established monthly. Anesthesiologists placed on reserve (versus regular duty) are paid an additional $1,000 if they are called to work, which usually happens the day before they’re needed. They get salaries but no extra compensation if not called. Overtime, which accrues most often if the schedule has underestimated time for regularly scheduled doctors to complete procedures, is compensated at $180 an hour.
Traditional staffing software helps limit explicit costs, such as those $1,000 payments and overtime fees, that arise when working with uncertain demand. But it doesn’t usually account for the implicit costs, such as paying salaries and benefits to idle physicians because there’s not enough work for them or the inconvenience to employees of being placed on an unused reserve list.
While doctors usually accept reserve duties as part of their jobs, many don’t appreciate repeatedly being put on call when not needed, the study explains. Reserve duty restricts what they can do outside of the hospital, including earning more money elsewhere.
Incorporating Explicit and Implicit Costs in the Model Saves Money
Using historic data from UCLA Medical Center, Rath and Rajaram develop a method to elicit implicit costs from past decisions. They then develop a large-scale optimization model, which incorporates explicit and the estimated implicit costs, along with uncertainty in surgical durations to determine the staffing schedule. When compared against the actual costs the hospital incurred, they found that the model’s plan reduced costs by about 16.5%, or $2.17 million on an annual basis, in explicit and implicit costs.
Other takeaways from the study might guide hospitals to more cost-effective operating room staffing, with or without a model. For example, the cost of not calling an anesthesiologist from the on-call list is “significantly more expensive” than actually calling them, according to the results. And the costs of idle time — of employing too many physicians — is substantially higher than the cost of overtime.
The findings suggest that those hands-on staffing managers are right: Implicit costs are too important to the bottom line to leave to an algorithm that doesn’t consider them.
Featured Faculty
-
Kumar Rajaram
Professor of Decisions, Operations and Technology Management
William E. Leonhard Chair in Management
About the Research
Rath, S. and Rajaram, K. (in press). Staff Planning for Hospitals with Implicit Cost Estimation and Stochastic Optimization. Productions and Operations Management.