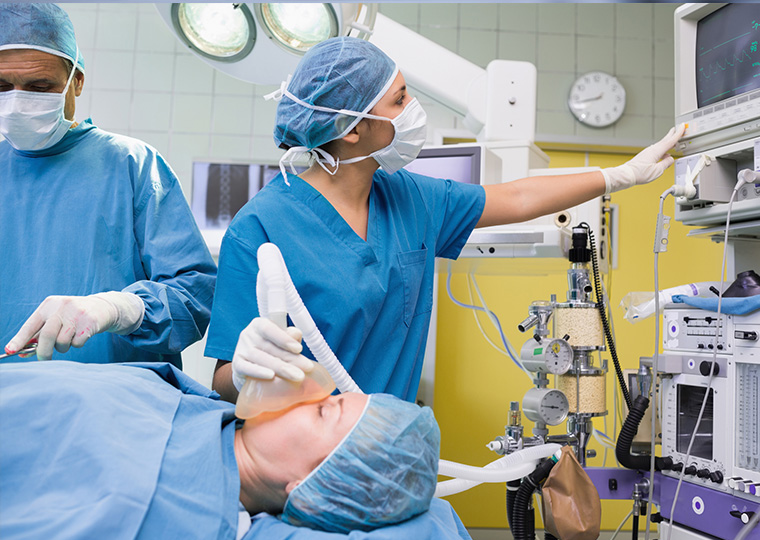
At the end of a night shift, empathy for patients’ hurting seems diminished
When dealing with a potentially life-threatening illness or injury, the best time to land at an emergency room is ASAP.
But there’s a subset of less critical situations where you may have more leeway to decide when to seek out treatment at an emergency room. And timing it right might help.
Opt In to the Review Monthly Email Update.
In a recent survey, nearly half of 1,425 ER workers said midmorning (6 a.m. to noon) was likely when you would get the best care, more than double those who recommended a late-night (midnight to 6 a.m.) visit.
A study published online in the Proceedings of the National Academy of Sciences suggests that for painful, but not life-threatening symptoms — e.g., debilitating back pain or a severe headache — there’s another reason to consider avoiding a late-night ER run: Your odds of not receiving a prescription painkiller are higher.
Hebrew University of Jerusalem’s Shoham Choshen-Hillel led a team of 11 other researchers, including UCLA Anderson’s Eugene M. Caruso, who studied more than 13,000 ER records across three hospital systems in Israel and the United States.
The team found that patients treated by a doctor late at night/very early morning — at the tail-end of a 26-hour night shift — were 20% to 30% less likely to be prescribed painkillers than patients who were treated by fresher doctors not working insanely long, circadian-crushing hours. This finding persisted even when the researchers accounted for a variety of factors, including patient self-reported levels of pain, the type of problem and differences in doctor specialty.
That lower prescription rate wasn’t some form of best-practice caution. The researchers found that during the late-night shift, doctors were more likely to under-prescribe based on “generally recommended” protocols of the World Health Organization.
Exhaustion Saps Empathy
At the end of the day, doctors are still human. And exhausted humans are never at their best. The researchers focused on how exhaustion might impact empathy, which is a vitally important trait for doctors when assessing pain levels.
As anyone who has been through this dance with a doctor knows, patients are asked to describe their level of pain (on a scale of 1 to 10) and doctors are then tasked with incorporating that subjective reporting into their clinical assessment.
In a warmup study to their analysis of hospital records, the researchers had 67 doctors complete a variety of tasks to get at their assessment of hypothetical patients’ pain level and gauge the level of doctor empathy lurking behind their pain assessment.
The doctors in this experiment who had just come off a 26-hour shift had “significantly” lower levels of empathy than doctors starting a regular shift in the morning. To be clear, neither group was well-rested, but the night-shift group was the most sleep-deprived, operating on an average of less than three hours of sleep, compared with nearly six hours for the control group.
In this study, the prescribing patterns among doctors in the two shifts showed no significant difference.
Exhaustion as Prescription for Under-Treating Pain
But when the researchers dove into the actual discharge records of thousands of ER patients, they did find that doctors working a 24-plus hour shift, were less likely to prescribe painkillers for patients they saw late at night/early morning, compared with doctors on a regular shift.
One of the discharge data sets covered 5,000 ER cases from an Israel health care system from 2014 through 2019.
Among patients seen during the day, half left with a prescription for a painkiller, compared with 39% of patients seen on the night shift. In an analysis from two other datasets (total of 13,482 patients), one from Israel and one from a Missouri health care system, a similar pattern arose.
As the graphic below shows, this prescription disparity persisted even when patients reported a high level of pain (between 7 and 10). Patients reporting a severe level of pain who were seen during the day were more likely to be given a painkiller, and an opioid, at that.
Painful Lessons
These findings should contribute to the debate around the efficacy of subjecting medical residents to crushing 26-plus hour shifts.
“We hope our findings inspire more work to weigh the benefits of shorter shifts with the unwanted consequences due to loss of education opportunities for physicians, greater workload and interruptions in the continuity of care,” the authors conclude.
In the meantime, to the extent you can control when to head to the emergency room, avoiding a middle-of-the-night visit may lead to better pain management.
Featured Faculty
-
Eugene Caruso
Professor of Management and Organizations and Behavioral Decision Making, Bing (’86) and Alice Liu Yang Endowed Term Chair in Teaching Excellence, Faculty Co-Director, Inclusive Ethics Initiative
About the Research
Chosen-Hillel, S., Sadras, I., Gordon-Hecker, T., Genzer, S., Rekhtman, D., Caruso, E.M., Clements, K.L., Ohler, A., Gozal, D., Israel, S., Perry, A. & Gileles-Hillel, A. (2022). Physicians prescribe fewer analgesics during night shifts than day shifts. Proceedings of the National Academy of Sciences, 119(27), e2200047119.